
HOW TO PASS YOUR CQC INSPECTION:
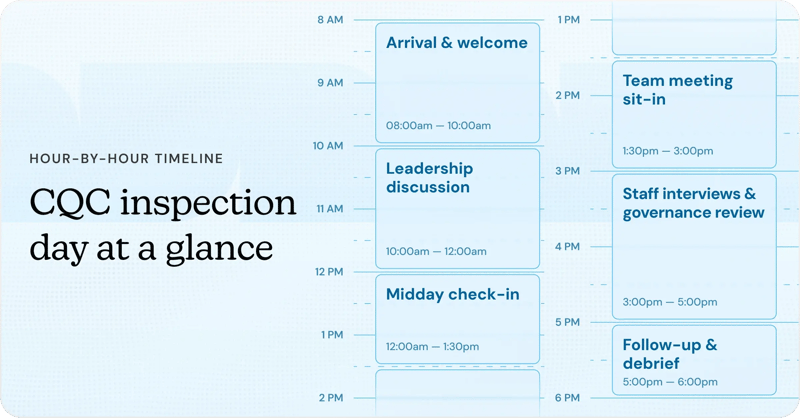
How CQC inspection day unfolds: An hour-by-hour guide
A full day of CQC inspections can be a daunting prospect, so sometimes it helps to break it down a little. This guide will help you prepare and present your practice with confidence, focusing on the evidence and environment at each stage.
| Gabi Ashton CQC Compliance Specialist, Let’s Make Lemonade |

8:00am: Arrival and welcome
Your inspection team will arrive at the beginning of the day, usually unannounced. There are some rare occasions where the inspection will be announced first. For instance, NHS GP practices are more likely to receive around two weeks’ notice by phone, unless the inspection is responding to a specific concern, but it’s pretty uncommon for most.
They’ll want to see how your practice operates in real life from the very first moment. The tone is set here: inspectors will notice how welcoming, safe and organised your environment feels.
These first impressions matter, so get the basics ready.
The prep:
- Make sure your reception area is clean, tidy and uncluttered. All staff on front desk duty should know how to greet inspectors, offer them a seat and provide refreshments.
- Ensure signage is clear and up-to-date, and that the area is accessible for all visitors, including those with disabilities.
- Have a printed or digital welcome pack ready with key documents: safeguarding contacts, emergency procedures, staff rota and practice contact list.
- Introduce the practice manager or senior staff members straight away. A friendly “good morning, let me show you where you can work today” goes a long way.
9:00am: Tour, logistics and introductions
It’s go time! In many inspections, the first formal part of the day isn’t a sit-down meeting, it’s a tour of the premises. This gives the inspector an immediate sense of how the practice works in real life.
They’ll often want to see the layout, understand the flow of patients and staff and get practical bearings: where key clinical and non-clinical areas are, where the fire exits and bathrooms are and where they’ll be based during the day. This first walkaround can also reveal a lot about safe environments, infection prevention, risk management and how well the service is organised.
Inspectors will want to ensure patients are aware CQC is on site and able to speak to them if they want to.
Next, they run through the plan for the day: who they’ll speak to, which areas they’ll review and whether anything needs to change due to absences, new starters or service pressures. A short catch-up with the registered manager and practice manager will also take place; several short meetings throughout the day usually works best as they’re busy.
The prep:
- Do a walkaround first thing. Check waiting areas, consulting rooms, staff areas and shared spaces.
- Think beyond appearances. Cleanliness matters, but so do practical details like clear exits, up-to-date notices, hand hygiene signage and safe storage.
- Make it easy for patients to engage. If appropriate, have a sign available letting patients or visitors know inspectors are on site and that they can speak to them if they wish.
- Flag any important context early. Let the inspector know if there are staff absences, new recruits, recent changes or anyone they should particularly speak to.
- Plan check-in points. It can help to agree short catch-ups with the practice or registered manager later in the day, so you’re not trying to answer everything on the fly.
10:00–11:00am: Leadership discussion and key context
Once the inspector has seen the site, they’ll often want to speak with the practice manager, registered manager or leadership team.
This might require you to give a short presentation (about 5-10 minutes), but every inspector is different. Sometimes it’s more of a conversation: what’s working well, where the challenges are, any recent incidents or complaints, staffing changes and anything important they should understand about the service. It’s also an opportunity for you to ask any burning questions you have about the day ahead.
Your inspector then might take some time to finalise the plan and perhaps do a second lap around the site to check anything they might have missed the first time. Give them the space to do so.
The prep:
- Have a short overview ready: patient population, services you provide, your approach to patient safety, staffing and recent improvements.
- Be honest about challenges and explain what you’re doing about them.
- Mention any recent significant events, complaints or new recruits.
- Keep it clear and practical rather than overly polished.
- Have ready any questions that’ll help you prepare for the day.
11:00am–12:00pm: Reception observation and early evidence review
The late morning is often a useful time for inspectors to observe reception and front-of-house teams, especially when the service is busy. This might be stressful for that team, but it can tell your inspector a lot about confidentiality, privacy, dignity, triage, signposting, teamwork and how staff support patients in real time.
It’s also useful to see ‘live’ how effective your systems are. If patients are willing, your inspector may speak to them about their experience, ideally pre- and post-appointment.
Alongside this, they may start reviewing some early evidence or asking for documents.
The prep:
- Brief reception staff and empower them on the basics: confidentiality, escalation and signposting etc. Make sure they feel confident using your practice management system.
- Make sure patient privacy is protected in practice, not just in policy.
- Have key documents easy to access if requested.
- Reassure staff that natural, honest answers are best.
12:00–1:30pm: Midday pause and check-in
And that’s lunch! Around midday, inspectors will usually take a short pause to reflect on what they’ve seen so far. This is often followed by a quick catch-up with the practice manager or registered manager to discuss any questions, early themes or practical changes to the afternoon plan. If there are any immediate risks or concerns, these will be raised.
The prep:
- Use the pause to gather any evidence still outstanding.
- Keep key leads available in case questions come up.
- Treat this as a practical check-in, not a formal feedback session.
- Listen for themes the inspector may be returning to.
1:30–2:30pm: Team meetings, MDTs or live working in action
If there’s a team meeting, multidisciplinary meeting or operational huddle happening, your inspector might want to sit in. This gives them a live view of teamwork, compassionate leadership, inclusive decision-making, staff knowledge, treatment and risk assessment planning and how well governance happens in practice.
The prep:
- If you have a suitable meeting, plan for it in advance and brief those in the meeting beforehand.
- Make sure agendas, minutes and actions are easy to show.
- Let the team be themselves; inspectors want to see real working practice.
- Don’t worry if there isn’t a formal meeting; the slot may simply be used differently.
2:30–3:00pm: Patient voice and service experience
This part of the day may include conversations with patients, visitors or your Patient Participation Group (if you have one arranged). Inspectors want to understand whether patients feel listened to, whether information is accessible and how the practice responds to feedback. These conversations can be completed face-to-face or remotely depending on the preferences of the group.
The prep:
- If patients are invited to speak, make sure it feels voluntary and comfortable.
- If you have a PPG, organise this in advance where possible.
- Be ready to show not just how feedback is collected, but how it leads to improvement.
- Think about accessibility and equity in how patients experience your service.
3:00–4:30pm: Staff interviews and governance deep dive

This is often where the inspection gets more detailed. Inspectors may speak to clinical and non-clinical staff, revisit questions from earlier and work through governance evidence in more depth.
They may focus on areas like safeguarding, infection control, complaints, recruitment, training, significant events and leadership.
The prep:
- Staff should understand the basics of their role and where to find policies.
- Reassure them it’s okay to say, “I’m not sure, but I know where to check.”
- Have someone available to support document requests quickly.
- Bring your improvement work to life with audits, learning and examples.
4:30–5:00pm: End-of-day feedback
Towards the end of the day, inspectors will usually share what they’ve seen so far. This won’t be the final report, but it will give you a sense of strengths, any immediate concerns and whether they need further evidence after the visit.
The prep:
- Take detailed notes.
- Ask for clarification if anything is unclear.
- Respond positively if concerns are raised.
- Be ready for follow-up requests after the inspection.
After the inspection: what happens next
Once the on-site visit ends, the process might still continue. Inspectors often review their notes afterwards and might follow up with extra questions or evidence requests in the days that follow. You can also follow up with any questions you may have; some inspectors might give you a couple of days to get these sent over. Some inspections may also continue remotely or into a second day if the inspector didn’t manage to complete all their interviews.
The prep:
- Hold a quick team debrief to review what went well and any issues raised.
- Gather any extra evidence or documentation requested.
- Don’t panic if more questions come through, that’s completely normal.
- Thank your team. Inspection day is tough! And it takes a lot to get there, so make sure you acknowledge everyone’s effort during the day.
CQC inspections are about showing how your practice really works, and the more prepared, open and organised you are, the easier that becomes.

Gabi Ashton has worked in the Health and Social Care sector for over 15 years, in CQC Regulated Services and as a CQC inspector. Her experience on both sides of CQC has given Gabi valuable insights into why and how services are rated from Inadequate to Outstanding.
Gabi now runs Let’s Make Lemonade, specialising in CQC compliance with the aim of driving improvements for providers across the health and social care sector. To work with Gabi on a mock inspection, visit Let’s Make Lemonade.
Get insights to your inbox every month. Sign up to The Pulse.



.webp?width=380&height=201&name=Ongoing%20requirements%20(1).webp)